This toolkit has been created through a collaborative effort between SHOT, the Royal College of Pathologists (RCPath) Transfusion Specialty Advisory Committee, and representatives from across the UK. The toolkit has been endorsed by all the UK national transfusion committees including the National Blood Transfusion Committee (NBTC), Northern Ireland Transfusion Committee (NITC), Blood Health National Oversight Group (BHNOG), and Scottish National Blood Transfusion Committee (SNBTC).
Major haemorrhage simulation toolkit
Click below to access the complete major haemorrhage simulation toolkit.
Major haemorrhage simulation toolkitBelow are the key highlights from the major haemorrhage simulation toolkit.
Summary
The Major Haemorrhage Simulation Toolkit helps healthcare teams improve safety and readiness when managing major haemorrhage (MH). Developed in line with UK patient safety guidance, it promotes realistic, multidisciplinary simulation training involving clinical, laboratory, and support staff.
- The toolkit explains different types of simulation, from scenario-based to virtual and augmented reality and offers practical guidance on planning, delivery, and debriefing
- It recommends regular, inclusive training that reflects real clinical environments to strengthen teamwork, communication, and system reliability
- By combining structured practice with clear follow-up through debriefs, audits, and action plans, the toolkit supports continuous learning and improvement
Its ultimate goal is to standardise MH response, reduce delays and errors, and improve outcomes for patients experiencing major haemorrhage.
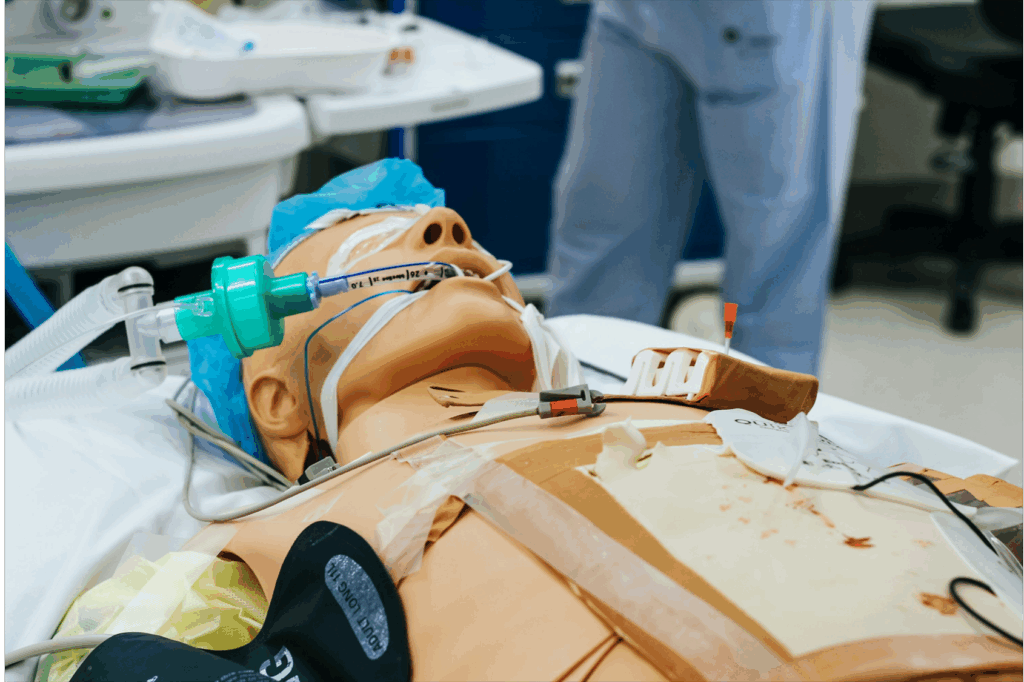


The resources and materials provided are intended to support local simulation training exercises. Their use is not mandatory, and we recognise that this is not an exhaustive list of available tools or approaches. Staff are encouraged to adapt, modify, or replace the scenarios and resources as needed to best meet their local requirements, operational needs, and professional judgement.
In January 2022, a UK-wide Patient Safety Alert reiterated the urgent need for hospitals to review their transfusion procedures and embed safe practices. Among its key recommendations was the implementation of regular simulation training in the management of major haemorrhage, with the aim of enhancing patient safety through system-level preparedness.
Simulation training

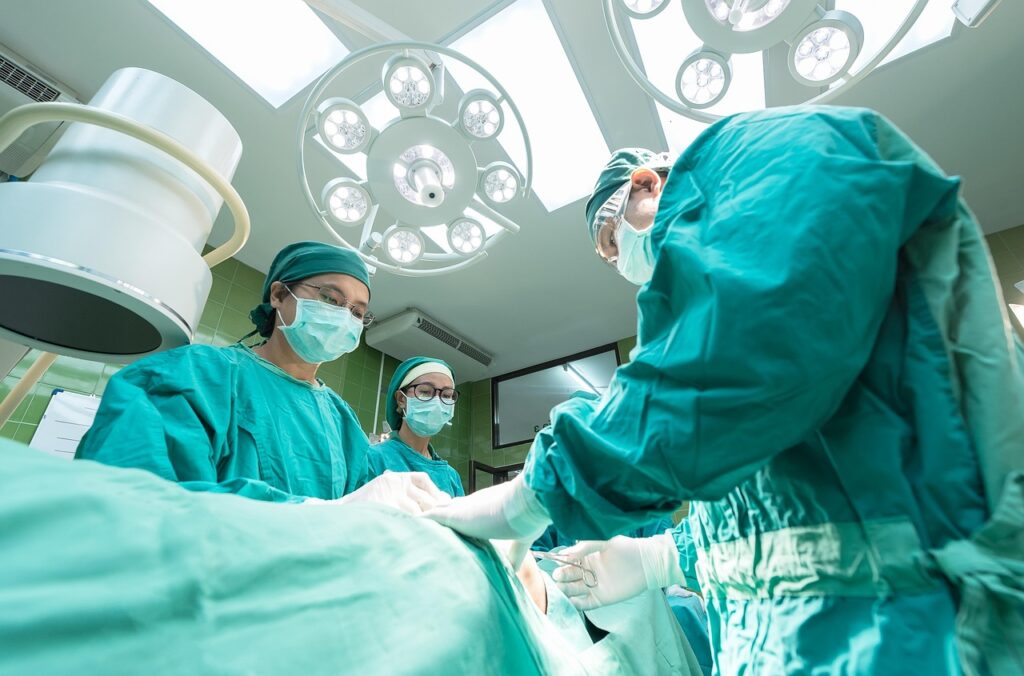
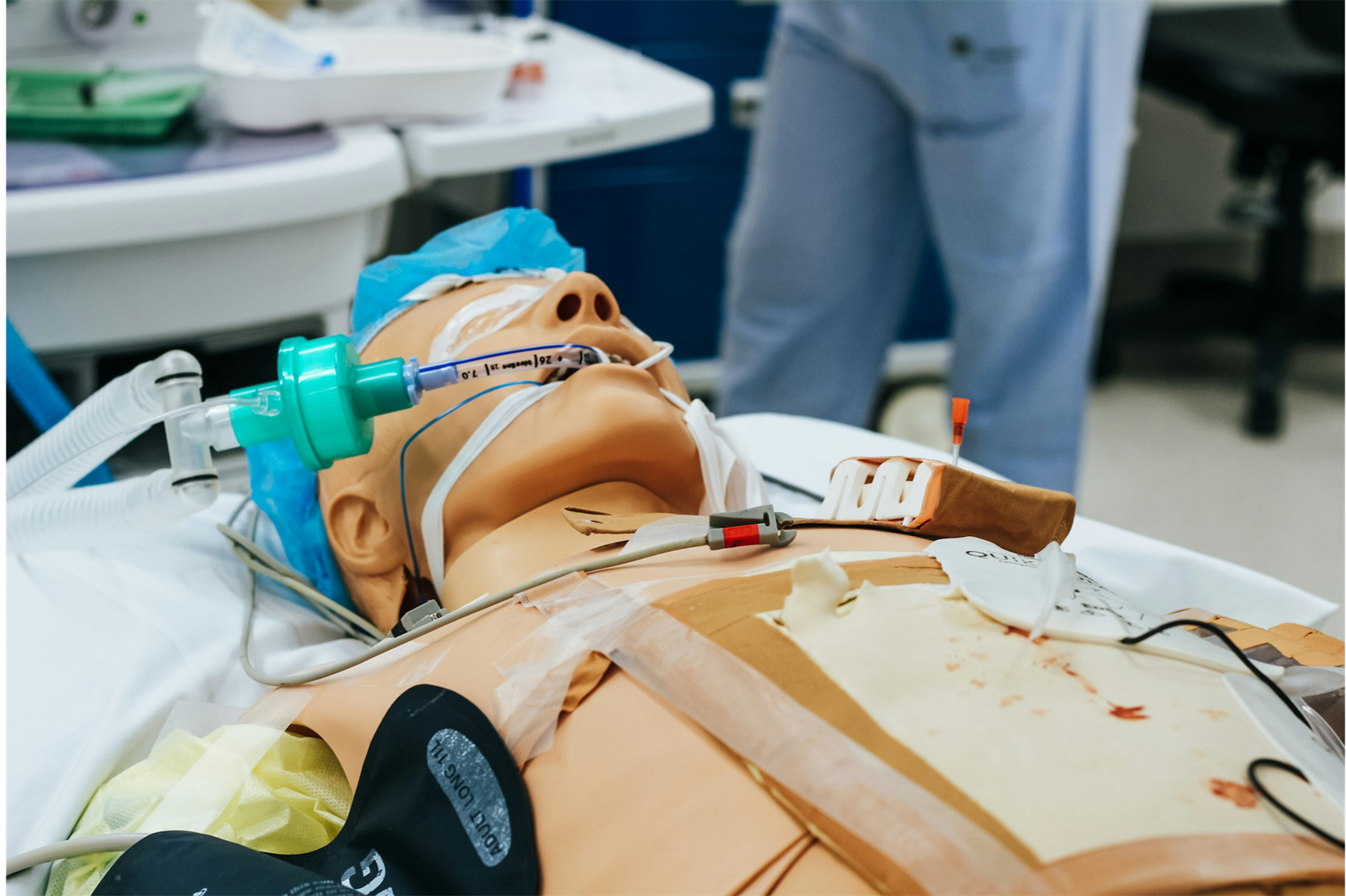
Key personnel
Managing major haemorrhage is a multidisciplinary task that requires the seamless coordination of clinical, laboratory, and logistical teams (such as porters). Effective simulation must therefore involve all key players in the transfusion pathway. Including laboratory staff and portering services ensures a truly end-to-end systems test, revealing weaknesses that traditional, clinically focused training may miss. This section outlines who should be involved in simulation sessions and why their role is critical to patient safety and protocol adherence. These are not prescriptive and may vary dependant upon staff availability and skill mix. Example staff groups are displayed below in alphabetical order.
By engaging the full multidisciplinary team, simulation exercises not only improve individual performance but also strengthen communication, coordination, and system resilience in the management of major haemorrhage.
Frequency of training
Post-simulation activities and actions
Simulation is only valuable if it drives learning and improvement. Post-simulation activities such as structured debriefs, audits, and action planning are critical for embedding change, improving safety, and closing the loop on systems improvement. This section discusses how to capture learning from simulation events, engage staff in meaningful reflection, and use data to guide service development and education strategies. Example debrief documents and external resources are outlined in the Resources section below.

Resources
To support the implementation of major haemorrhage simulation training, this toolkit includes a range of resources from clinical scenarios to practical tools for mock transfusion. These materials are designed to be flexible and adaptable across different hospital environments. They also include guidance on incorporating laboratory systems, setting up simulated patients in LIMS, and sourcing appropriate equipment. This section provides a consolidated list of these resources and relevant links for further support.
The resources and materials provided are intended to support local simulation training exercises. Their use is not mandatory, and we recognise that this is not an exhaustive list of available tools or approaches. Staff are encouraged to adapt, modify, or replace the scenarios and resources as needed to best meet their local requirements, operational needs, and professional judgement.
Simulation scenario templates
These templates include:
- Blank template for major haemorrhage simulation scenario
- Gastrointestinal bleed simulation scenario
- Surgical bleed simulation scenario
- Major obstetric haemorrhage scenario
- Neonatal haemorrhage scenario
- Case study of worked example neonatal haemorrhage
Click below to access all the major haemorrhage simulation scenarios
MH simulation scenariosBlood bags for major haemorrhage simulation
Click below to access the blood bags for use during MH simulation
MH simulation blood bagsGenerating mock patients for major haemorrhage simulation
Click below to access a document detailing considerations when creating mock patients for simulations.
MH simulation creating mock patientsDebriefing tools and resources
Click below for a debrief template and external debriefing resources.
MH simulation debrief MH simulation further resourcesAll images used are referenced within the major haemorrhage simulation toolkit document.
Collaborative groups involved in the creation of this document and associated resources:





Feedback
SHOT would appreciate any feedback, comments or suggestions for this Major Haemorrhage simulation toolkit. Please contact the team via this link to submit your suggestions.